I. Introduction
Joint pain is a common medical issue that affects millions of people all over the world. Pain in a joint indicates irritation, soreness, or inflammation in that joint. Joints are the connections between bones that allow for motion and flexibility. Joint pain, no matter how mild or severe it is, may significantly impact a person’s daily life. It may be effectively diagnosed and treated if the underlying reasons are identified and addressed.
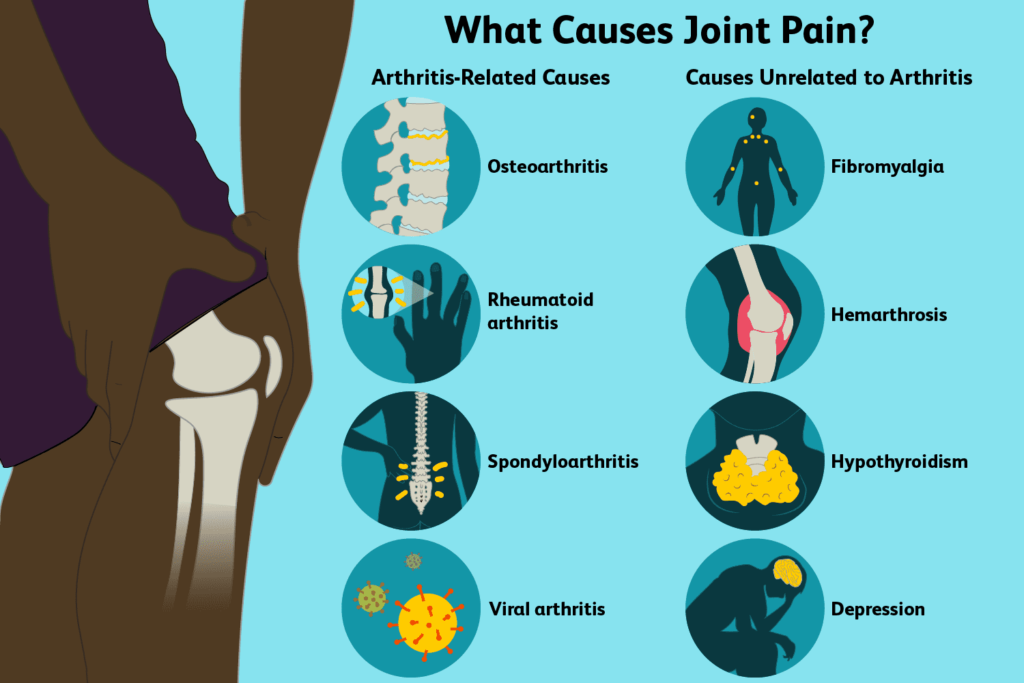
II. Causes of Joint Pain
1. Osteoarthritis:
Osteoarthritis knee is the most prevalent kind of arthritis and a major source of joint pain, especially in the elderly. As we age, the cartilage that normally cushions our bones at their ends wears away, leading to painful bone-on-bone rubbing. Among the joints that might feel the effects of this are the knees, hips, limbs, and pain in lumbar spine.
2. Rheumatoid Arthritis:
The synovium (the lining of the membranes that surround the joints) is attacked by the body’s immune system in rheumatoid arthritis, an inflammatory illness. Because it damages cartilage and bone, prolonged inflammation may lead to joint discomfort, swelling, and even deformity. Joints of the hands, wrist pain, and ankles are among those most commonly affected by rheumatoid arthritis.
3. Gout:
The great toe is the joint most usually affected by gout, a kind of arthritis marked by sudden and intense joint pain. Uric acid crystals build up in the joints, causing inflammation and unbearable agony. Gout attacks may be precipitated by consuming or drinking anything that causes an increase in the body’s uric acid levels.
4. Bursitis:
Inflammation of the bursae, which are fluid-filled sacs that act as cushions and lubricants for joints, is known as bursitis. Overuse, repeated motion, or injury may all lead to bursitis, which causes pain and sensitivity in the joints in a localized area. Involvement of the frozen shoulder, elbow, hip, and knee is common.
5. Tendinitis:
Inflammation or irritation of the tendons, the fibrous ligaments connecting muscles to bones, is known as tendinitis. Joint pain and soreness are symptoms of tendinitis, which may be brought on by either overuse or repeated motions or by sudden injury.
III. Symptoms of Joint Pain
Joint pain may have a wide range of symptoms depending on the underlying reason. The most often-seen symptoms of joints pain are:
1. Swelling:
Edema, brought on by joint inflammation, manifests as a hefty or puffy increase in the joint’s circumference.
2. Stiff or Enlarged Joint:
Painful or limited range of motion due to joint stiffness or enlargement. Arthritis and other psychological disorders may cause the joint to swell and even distort somewhat.
3. Numbness:
Numbness or pain in the affected region may be the consequence of nerve compression or inflammation in the area surrounding the joint.
4. Painful Movement:
In most cases, moving around makes joint pain worse. Walking, climbing stairs, or doing repeated actions may all bring on or exacerbate the pain.
5. Difficulty Bending or Straightening the Joint:
When you have joint pain, your range of motion may decrease. Further, making the joint become stiff and resistant to motion, it might be difficult to fully bend or straighten the afflicted limb.
6. A Red, Hot, and Swollen Joint:
Rheumatoid arthritis and gout are two examples of inflammatory disorders that may cause the affected joint to become red, hot, and swollen. The inflammation itself is what causes the heat, while the increased blood flow to the region is what causes the redness.
IV. Diagnosis of Joints Pain
Integration of patient history, physical examination, imaging examinations, blood tests, and sometimes joint aspiration (arthrocentesis), are required to determine the source of joint discomfort. Each of these diagnostic procedures contributes unique data that help doctors zero in on the root of joint pain.
1. Medical History
The medical history of the patient is the first step in determining the cause of joint discomfort. The patient should be prepared to answer questions regarding the beginning of symptoms, the location and level of pain, the variables that increase or relieve pain, any past injuries or medical disorders, and any family history of joint difficulties.
2. Physical Examination
A thorough physical evaluation of the injured joint and its surrounding components is necessary. The doctor will check for swelling, redness, warmth, soreness, and any abnormalities in the joint. They’ll also check the patient’s overall musculoskeletal condition and range of motion in the affected joint.
3. Imaging Studies
Imaging scans are often used to analyze the joint’s interior anatomy and detect any abnormalities. Common diagnostic imaging procedures for arthritic joints include:
- Fractures, joint degeneration, and other structural abnormalities in the joint may be detected with the use of X-ray pictures since they offer thorough views of bones.
- By using strong magnets and radio waves, MRI can capture detailed pictures of soft tissues including ligaments, tendons, and cartilage.
- Doctors even use Musculoskeletal USG, a tool that helps in providing real-time images. It is a high-frequency sound wave that is used to capture images of soft tissues.
- Bone and soft tissue cross-sectional pictures may be obtained effectively with CT scanning. They may be helpful in further assessing the architecture of joints in certain circumstances.
- Joint Aspiration (Arthrocentesis)
Ultrasound guided aspiration (arthrocentesis) of a tiny amount of fluid from the afflicted joint may be performed in certain cases. In order to diagnose an infection, inflammation, or crystal formation (as in gout), the fluid must first be analyzed.
V. Treatment of Joints Pain
Radiofrequency Ablation (RFA)
Radiofrequency ablation (RFA) is a minimally invasive surgery that uses radiofrequency radiation to selectively inactivate nerves that are responsible for referring pain from an injured joint.
Nerve block
A nerve block is an injection of an anesthetic or anti-inflammatory medicine into or near the nerves that supply the painful joint. Short-term pain relief is achieved because the nerve is briefly prevented from delivering pain signals.
Genicular Artery Embolization (GAE)
Genicular artery embolization (GAE) is a cutting-edge method for relieving bending knee pain caused by osteoarthritis. This technique involves injecting tiny particles into the blood vessels that feed the knee joint pain, cutting off blood supply and relieving pain and inflammation.
PRP therapy
Platelet-Rich Plasma (PRP) Therapy involves drawing a tiny amount of blood, processing it to concentrate the platelets and growth factors, and then injecting the resulting PRP into the injured joint.
Growth factor
Proteins called growth factors are used in growth factor treatment to promote healing and cell development. Injections or other administration techniques are available for this therapy, which aids in the repair of joint tissue and decreases inflammation.
VI. When to Seek Medical Attention
Prompt medical assessment may lead to early identification and treatment of the underlying causes of joint pain, which can range in severity from mild to severe. Do not disregard swelling, inflammation, or immobility in the joints if they are already painful. In addition, getting medical attention right away is essential whether you have a fever, have been recently injured, or have widespread symptoms. Joint pain may significantly limit a person’s quality of life, but if caught and treated early, it can be eliminated along with the associated symptoms. Keep in mind that enhancing joint health and overall quality of life requires prompt medical attention.
VIII. Conclusion
Joint pain may limit a person’s motion and reduce their quality of life, which can exacerbate their existing physical and mental illnesses. If you’re experiencing joint pain, it’s crucial that you see a doctor to obtain a precise diagnosis and individualised treatment plan.
Restoring joint function and avoiding additional injury may reduce joint pain and enhance the quality of life with early management. If joint pain lasts a long time or becomes worse, it might significantly lower a person’s standard of living. When joint pain lasts more than a few days or becomes intolerable, it’s time to see a doctor. Long-term joint health and overall health may be improved by prompt diagnosis and treatment.