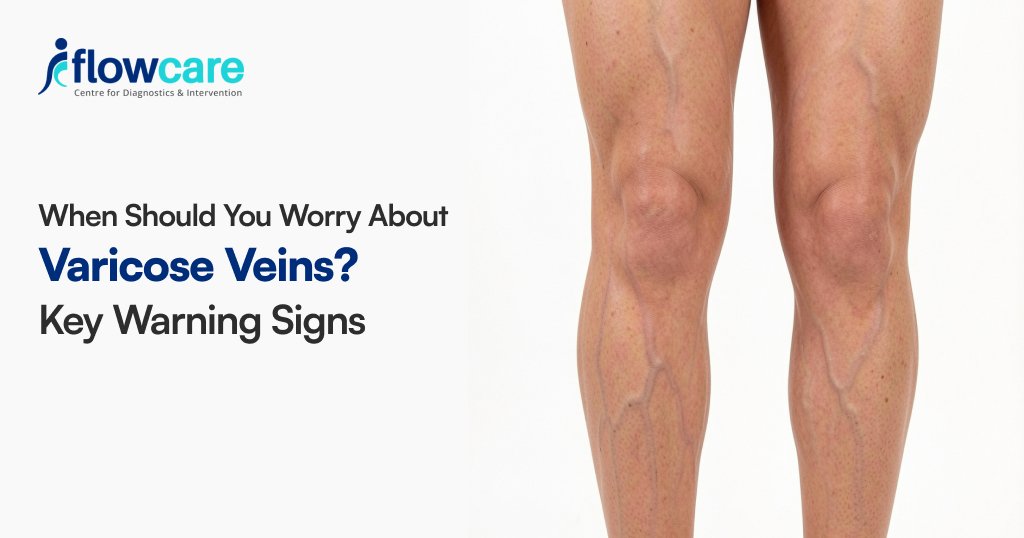
When Should You Worry About Varicose Veins? Key Warning Signs
Do you feel a dull aching pain in your legs accompanied by mild swelling in your ankles or feet after a long day of standing or sitting?
That might not be due to exhaustion but rather a deeper issue that you might have been ignoring.
This article explains a simple three-level urgency framework to help you understand where your symptoms fall and when you should seek medical attention.
What are Varicose Veins?
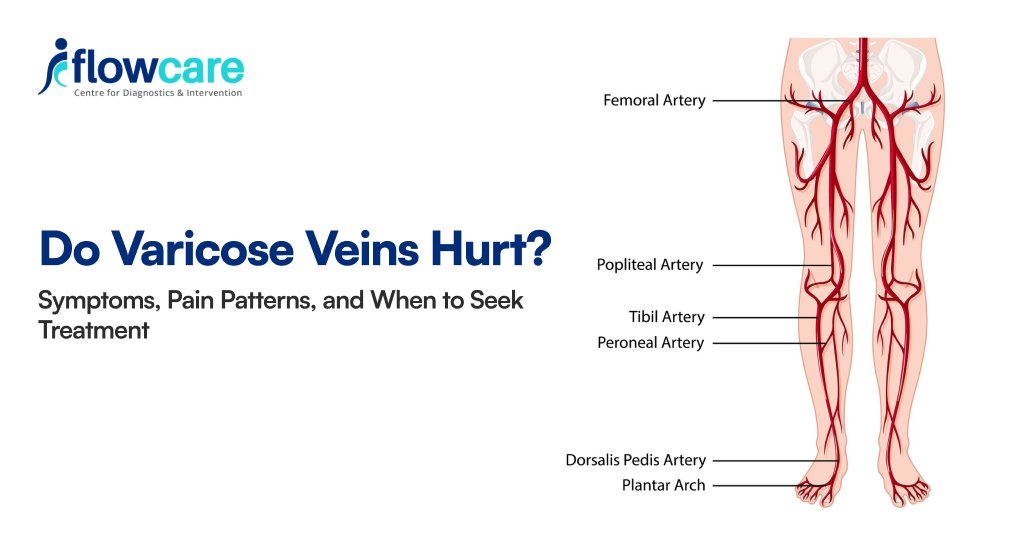
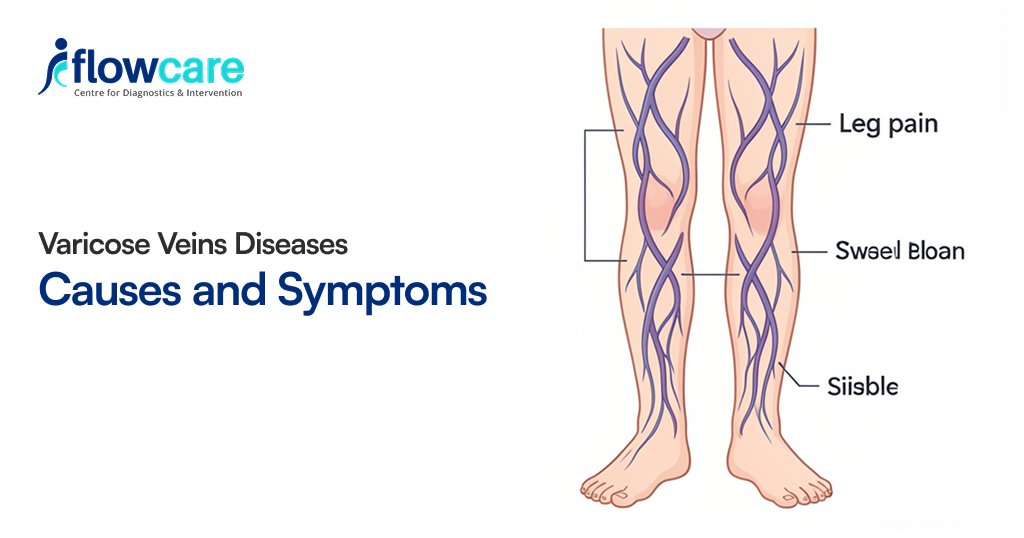
Varicose veins are enlarged, bulging veins that occur due to valve dysfunction in the veins, causing blood to pool instead of flowing properly toward the heart.
They most commonly affect the veins of the legs, especially in people with desk jobs or those who stand for long hours, such as doctors, teachers, or retail workers.
A 3-Level Signs and Symptoms Framework for Varicose Veins
Not all varicose vein symptoms are equally urgent. Here is a quick overview before we examine each level in detail.
| Level | Symptoms | What it Means | Physical Changes |
| Level 1 | Mild leg heaviness, visible veins | Early symptoms: cosmetic concern becoming medical | Small bulging veins or spider veins |
| Level 2 | Pain, swelling, itching | Disease progressing: skin & tissue being affected | Skin darkening, thickening, visible enlarged veins |
| Level 3 | Non-healing wounds, severe swelling | Active complication: urgent or emergency situation | Venous ulcers, severe skin damage |
Source: pmc(1)
Read on for the full breakdown of what each sign means, why it matters, and exactly what to do about it.
Level 1: Early Symptoms of Varicose Veins
Heavy, Achy, or Tired Legs by Evening
Many people live with Level 1 symptoms, such as mild pain, heaviness, or stiffness in the legs, especially after standing or sitting for long hours.
It is not always just fatigue or ageing. It may indicate that the valves in your veins are beginning to weaken.
Here is what happens, Healthy veins act like a pump that pushes blood upward against gravity toward the heart. When these valves become weak, they begin to leak.
Blood pools in the lower leg instead of travelling upward, raising pressure inside the vessel and causing the surrounding tissue to feel congested and fatigued.
Ankle or Lower Leg Swelling That Goes Down Overnight
During clinical practice, many patients complain about leg swelling in the evening. This is classic venous oedema, one of the symptoms of varicose veins.
High pressure from the varicose veins forces fluid through the vessel walls and into the surrounding tissue.
When you elevate your legs at night, gravity helps drain it which is why the swelling goes down in the morning and the cycle repeats the next day.
If you notice this pattern regularly, it is advisable to consult a vascular specialist.
Itching or Burning Over a Vein
If you have a patch of skin that itches or burns consistently and there is mild discolouration of the skin this is most likely not eczema or dryness.
Increased venous pressure irritates small nerve fibres in the surrounding skin.
The danger of ignoring it: constant scratching damages already-fragile skin, increasing the risk of skin breakdown and future ulceration.
If itching does not improve with moisturisers, the underlying venous problem should be evaluated.
Skin Near Your Ankle Is Changing Colour
Brown, rust-coloured, or reddish-purple patches appearing near the ankle are a definitive sign that venous disease has been progressing silently.
Skin colour changes usually indicate progressing venous disease and should be evaluated by a doctor.
Night Cramps or Restless Legs
Painful night cramps, especially in the calf muscles can be caused due to venous insufficiency. Pooled blood causes a disruption of oxygen and carbon dioxide in the tissues.
This can trigger involuntary muscle contractions and nerve irritation.
These symptoms are often mistaken for vitamin deficiency or dehydration, when the underlying cause may be vascular.
Book a Routine Appointment If You Have Any of These:
- Legs that feel heavy, achy, or tired most evenings
- Ankles that swell during the day and deflate overnight
- Persistent itching or burning directly over a vein
- Brown or rust-coloured skin patches near the ankle
- Regular night cramps or restless legs without another explanation
- Varicose veins that are visibly growing or multiplying over months
Level 2: Symptoms that Lead to Structural Changes
These symptoms cause the skin and fat around the affected veins to break down under sustained high pressure.
At this stage, the window for simple treatment is narrowing and the risk of developing a venous ulcer becomes real.
Here are some signs you may notice while evaluating your symptoms.
Skin That Feels Hard, Tight, or “Woody”
If your skin above the ankle seems hard, firm, or thick this is called lipodermatosclerosis.
This is a condition where fat and connective tissue gradually harden due to long-standing venous hypertension.
Patients often describe the feeling as if the lower leg is tightly wrapped or constricted.
In advanced cases the shape of the leg changes to an inverted bottle shape meaning narrow at the ankle, swollen above it.
White, Porcelain-Like Patches Near the Ankle (No Wound)
The condition is called atrophie blanche, it is a small white patch surrounded by visible red vessels (broken capillaries), mostly near the ankle or lower leg.
These are not scars from the previous injury, these are a result of blood flow disruption in the cells which has led to cell death.
The skin becomes extremely fragile and may break down with minimal trauma in such cases healing is poor due to altered blodd supply and can lead to ulcers.
Red, Weeping, or Crusty Skin on the Lower Leg (Venous Eczema)
It is one of the most frequently misdiagnosed condition often mistaken as a fungal infection or contact dermatitis when the real cause is elevated venous pressure.
This is how you can differentiate between a venous eczema and other skin disease,venous eczema often recurs in the same location around the ankle or the lower leg.
This does not respond to topical treatments and if ofent accompanied by other symptoms like swelling, varicose veins, or discolouration.
Long-term treatment requires addressing the underlying venous insufficiency.
A Vein That Has Become a Hard, Red, Tender Cord
In this condition a clot forms inside the vein leading to inflamation. Upon evaluation the area seems firm with red surface, warm and tender to touch, called superficial thrombophlebitis.
While this is a supreficil condition but is a risk factor for deep vein thrombosis (DVT).
Deep vein thrombosis (DVT) occurs when a clot forms in the deep veins, usually in the legs, causing pain and swelling.
In some cases the clot can break off and travel to the lungs causing breathing problem.
This can occur in 4.64% –41.7%(2) of cases.
See a Doctor Within Days If You Have:
- Skin around the ankle that feels hard, tight, or woody to the touch
- White or ivory patches near the ankle (no wound but fragile skin)
- Persistent red, weeping, or crusting skin on the lower leg
- A varicose vein that feels like a firm, tender, red cord
- A vein that has suddenly darkened, enlarged, or become painful without traum
Level 3: Symptoms that Need Immediate Medical Attention
This is a condition where delayed action can lead to serious harm.
Varicose Veins Bleeding
Bleeding from varicose veins is uncommon but can occur, bleeding can lead to serious complications.
Let’s understand what a person should do in such cases
1: Lie down immediately, do not sit or stand, gravity is your enemy at this point hence, lie down.
2: Elevate your legs above the level of your heart.
3: Apply gentle pressure with a clean cloth and hold it until the bleeding stops.
4: Once the bleeding stops, go to the doctor immediately because vessel wall has been breached and will bleed again without definitive treatment.
One Leg Suddenly Swells, Hurts, or Turns Red: Possible DVT
Deep vein thrombosis can sometimes occur in people with long-standing varicose veins diseases.
People with varicose veins carry a elevated baseline risk of DVT.
The risk rises during periods of immobility long-haul travel, surgery, hospitalisation, or prolonged bed rest.
Chest Pain, Breathlessness, or Coughing Up Blood
This condition occurs when a clot from the leg breaks and travels to the lungs, causing a pulmonary embolism.
Symptoms include sudden sharp chest pain, unexplained breathlessness, a rapid heart rate, feeling faint, or coughing up blood.
These symptoms can follow leg swelling or appear without warning.
A Leg Wound That Has Been Open for More Than 2 Weeks
A venous ulcer is an open woud caused by years of elevated venous pressure breaking down the skin.
These wounds suffer from chronic poor circulation and reduced oxygen supply, which delays healing.
They can persist for months or years, and carry a significant risk of infection (cellulitis), which can progress to systemic sepsis.
Treating only the wound surface without correcting the underlying venous reflux is rarely effective.
When the faulty veins are treated, healing improves significantly, and most ulcers close within a few weeks to months.
Conclusion
Varicose veins are a treatable medical condition and should not be considered a permanent problem that one has to live with.
With advances in vascular care, treatment has become faster, safer, and far more effective than before.
Modern minimally invasive procedures can close the faulty veins, restore proper blood flow, and significantly reduce symptoms.
Most treatments are performed as day-care procedures, usually taking less than an hour and requiring little to no downtime.
Patients are usually able to walk immediately after the procedure and return to their normal routine within a few days. The key, however, is timely evaluation.
When varicose veins are treated early, the treatment is simpler and the risk of complications such as skin changes or venous ulcers can be prevented.
FAQs
Can you get DVT from varicose veins?
Yes, deep vein thrombosis can occur in patients with long standing varicose veins. Studies have reported that the risk may be around 3–5 times higher, particularly in the first few years after diagnosis. (3)
What are the main causes of varicose veins?
Varicose veins occur when the valves in the veins weaken or stop working properly, causing blood to pool in the veins.
Common causes and risk factors include genetics, ageing, prolonged standing or sitting, pregnancy, obesity, hormonal changes, and a sedentary lifestyle.
What deficiency causes varicose veins?
Varicose veins are primarily caused by weakened vein valves and increased pressure in the leg veins, not by a specific vitamin deficiency.
However, deficiencies in certain nutrients such as vitamin C, vitamin E, and flavonoids may weaken blood vessel walls and reduce vein health, which can contribute to worsening symptoms.
A balanced diet that supports vascular health may help maintain healthy veins.
Latest treatment for varicose veins?
The latest treatment options for varicose veins are non-invasive. Here are some of the options available depending upon the case.
- Sclerotherapy
- Ultrasound guided sclerotherapy
- Endovenous laser ablation
- Radiofrequency ablation
- VenaSeal medical glue