Varicose Veins Disease: Causes and Symptoms
Varicose veins diseases affect 33% of adults between the ages of 18 and 64 years(1) yet many people find it difficult to figure out when to seek help.
This article gives a detailed overview about the disease, symptoms, modern treatment options, and more.
What is Varicose Veins Disease?
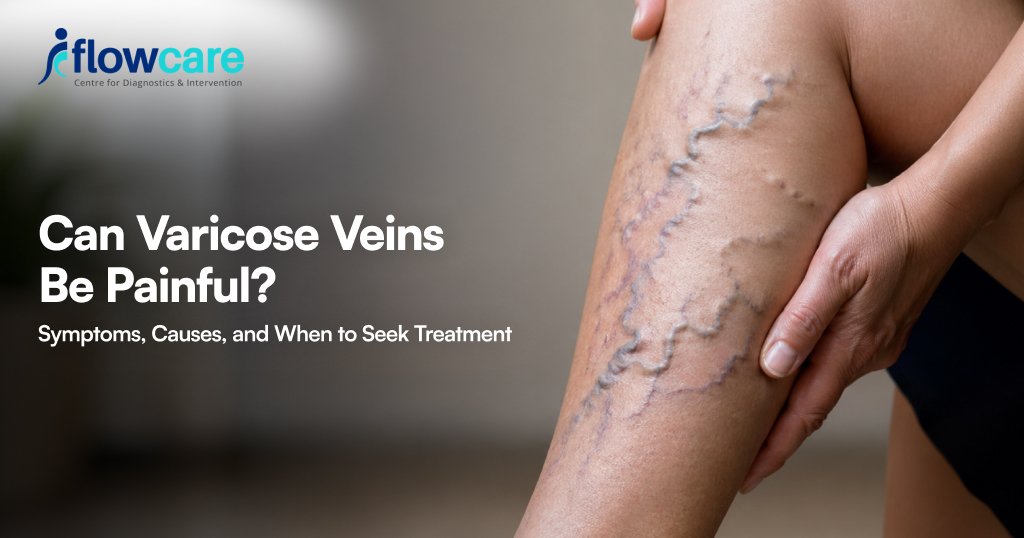
Varicose veins are enlarged, twisted, swollen veins that bulge beneath the surface of the skin, most commonly in legs and feet.
It is caused when one valve in the vein stops functioning properly, leading the blood to pool and veins to stretch and distort under pressure.
Varicose veins affect women more than men due to hormonal fluctuations that weaken the vein walls.
It is more than a cosmetic concern; it represents a more serious concern, i.e., venous insufficiency.
Is Varicose Veins Similar to Spider Veins?
The short answer is no. Though both the conditions represent the same similar causes, like weak vein valves, genetics, and pregnancy.
Spider veins (telangiectasias) are tiny, spider web-like vessels visible just under the skin. They’re smaller, flat, and generally cosmetic.
Both can occur together from valve dysfunction, but varicose vein disease carries much deeper symptoms and complications.
How Do Veins Work And What Goes Wrong?
To understand varicose veins diseases better, you must know how the veins work. Here is a basic overview.
Arteries carry oxygen-rich blood from your heart out to your body. Veins carry it back to a harder job, since blood must travel upward against gravity, particularly from the legs.
Inside these veins there are tiny valves that open to let blood move towards the heart, then close to prevent it from flowing back.
This mechanism is what keeps circulation moving efficiently when you stand, walk, or sit for long periods.
When the valves weaken, they fail to close and blood pools behind the faulty valves, leading to increased pressure and stretching of vein walls.
Eventually becoming the bulging, twisted vessel we recognize as a varicose vein.
Classification of Venous Varicosities: What Type Do You Have?
Varicose veins can be classified on the basis of size, depth, appearance, and how serious they are.
Think of it as a spectrum, and knowing where you fall on that spectrum helps set realistic expectations about symptoms, treatment, and urgency.
Classification by Size and Appearance
There are three main types:
- Spider Veins (Telangiectasias): The Smallest Type
What they look like: These look like tiny, thin red, purple, or blue lines often forming a sunburst, web, or branch-like pattern just beneath the skin’s surface.
They sit very close to the surface and are flat (you can’t feel them when you run your finger over them).
Size: Less than 1 mm in diameter
Location: They are most commonly seen on the legs, thighs, and face. On the face, they often appear around the nose or cheeks.
Usually no symptoms.
Spider veins are mainly a cosmetic concern, though some people notice mild burning or itching around them, especially after standing for long periods.
Think of them as the “warning light,” your body’s first signal that the venous system is under some stress.
- Reticular Veins: The Middle Ground
Appearance: larger than spider veins, with bluish-green veins that form a network or mesh under the skin.
They are flatter than varicose veins but clearly visible like a faint blue line on the back of your legs or behind your knees.
Size: Between 1 mm and 3 mm in diameter
Location: These appear on the back of the thighs, behind the knees, and on the outer leg.
Symptoms:
- Aching
- Itching
- Fatigue in the legs, particularly toward the end of the day.
- Varicose Veins: The Largest Type
The most commonly recognized type due to their bulging, twisted, or rope-like veins. These are easily palpable.
These veins are are blue, dark purple, or green, and often appear on the inner leg, calf, or behind the knee
Size: Greater than 3 mm in diameter
Location: Most often on the legs, particularly along the inner thigh, the back of the calf, and around the ankle.
Symptoms:
- Aching
- Heaviness
- Throbbing
- Itching
- Swelling
- Advanced cases: skin changes and ulceration
What Causes Varicose Veins Diseases?
Varicose veins are caused by a combination of genetic, lifestyle, hormonal, and other changes over time. Let’s understand those factors below in detail.
Primary Risk Factors
- Genetics and Family History
This is the most significantly considered factor responsible for varicose veins diseases. Studies reveal 85% (2) of patients have a positive family history.
Inherited connective tissue weakness and valve malformation are key mechanisms.
- Pregnancy
Varicose veins are common during pregnancy. Nearly 40% (3) of women are affected with this condition due to increased blood volume resulting from hormonal fluctuations.
This leads to direct pressure on pelvic veins. The risk increases with each subsequent pregnancy. Usually improve within 3–12 months postpartum.
Women are roughly twice as likely as men to develop varicose veins.
- Prolonged Standing or Sitting
Occupations requiring long hours on your feet like medicine, retail, and teaching increase venous pressure.
Similarly, prolonged sitting (desk workers, long-haul travelers) impairs calf muscle pump function, increasing risk.
- Age
Vein walls lose elasticity with age; this accelerates the development of valve incompetence, leading to blood pooling in the veins.
- Obesity
Excess body weight leads to an increase in abdominal pressure, leading to hindrance in blood return from the legs and raising pressure on vein walls.
Weight loss can slow progression, though existing varicosities typically require treatment.
- Prior Deep Vein Thrombosis (DVT)
A history of DVT can damage vein valves and alter flow patterns, leading to post-thrombotic syndrome, a condition that frequently includes secondary varicose veins.
⚠️ Risk Factor Summary
- High risk: Family history + obesity + prolonged standing + female sex
- Moderate risk: Age over 50, previous pregnancy, hormonal therapy
- Lower risk but meaningful: Sedentary lifestyle, previous DVT, constrictive clothing
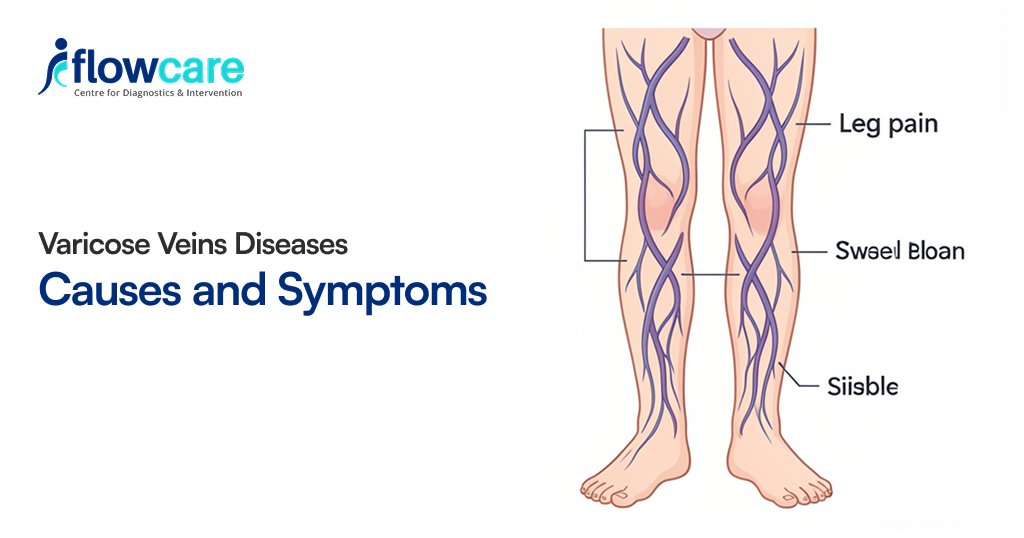
Varicose Veins Symptoms
Varicose veins are not always painful. Here are some of the common physical symptoms.
Common Symptoms Include
- Aching, heavy, or tired legs especially after standing
- Throbbing or burning sensation along the vein
- Itching around the vein (often mistaken for dry skin)
- Swelling of the ankles and lower legs, particularly by evening
- Muscle cramps, especially at night
- Skin discoloration—brownish patches near the ankle (haemosiderin staining)
- Restless leg sensations
Source: ncbi(4)
Seek Immediate Medical Attention If You Experience the Following:
• Sudden severe pain or swelling in one leg (possible DVT)
• A varicose vein that bleeds apply pressure and go to A&E
• Redness, warmth, and hardness along a vein (possible phlebitis)
• A leg ulcer that has been open for more than 2 weeks
How Are Varicose Veins Diseases Diagnosed?
Diagnosis begins with a thorough clinical history and physical examination, followed by duplex ultrasound, the gold standard for assessing venous anatomy and function.
The Clinical Examination
The specialist examines varicose veins in your feet while standing to maximize the venous filling, looking for skin changes.
Apart from this, the specialists also ask about symptoms, duration, family history, and any prior treatments.
Duplex Ultrasound: The Key Diagnostic Tool
Duplex ultrasound (DU) is one of the most commonly used diagnostic methods that detects the direction and velocity of blood flow in varicose veins diseases or chronic vein insufficiency.
This is a non-invasive, radiation-free, and painless test that takes 30–60 minutes.
When to See a Specialist?
- Visible varicose veins causing aching, heaviness, or swelling
- Skin changes around the ankle (discolouration, eczema, hardening)
- History of superficial or deep vein thrombosis
- A vein that has bled
- Any leg ulcer that has not healed within 2 weeks
- Varicose veins worsening during or after pregnancy
- Family history and early symptoms
What is Varicose Veins Treatment?
Treatment of varicose veins diseases is generally minimally invasive. Let’s know about it in detail below.
Conservative Management for Veins Varicosities
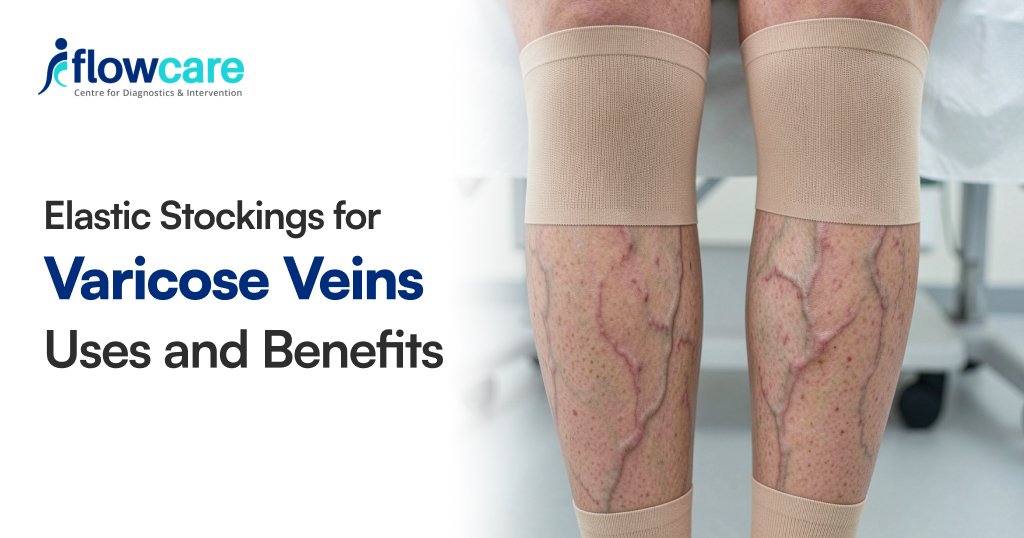
Compression Stockings
Varicose veins stockings are elastic garments designed to apply gentle pressure on legs, feet, and ankles. They help improve blood flow, reduce swelling, and prevent blood clots.
Always consult a professional before using compression stockings.
They do not treat or reverse varicose veins, but they are effective at managing aching, swelling, and fatigue, particularly during pregnancy or while awaiting treatment.
Lifestyle Modifications
Lifestyle changes will not eliminate the already existing issues, but the following measures can help slow progression, prevent relapse, and reduce symptoms:
- Regular walking and exercise to activate the calf muscle pump
- Leg elevation when resting (feet above heart level)
- Weight management
- Avoiding prolonged standing or sitting without movement breaks
- Avoiding tight clothing around the groin or waist
Minimally Invasive Treatments for Varicose Veins
- Endovenous Laser Ablation (EVLA / EVLT)
This treatment is ultrasound-based and is great for small varicose vein disease.
A thin laser fiber is inserted into the affected vein under local anesthesia, delivering heat energy that closes the vein from within.
The procedure takes 30–60 minutes, and patients are able to walk out and return to normal activities within 1–2 days.
Patients walk out and return to normal activities within 1–2 days.
- Radiofrequency Ablation (RFA)
This is very similar to EVLA; RFA uses radiofrequency energy instead of laser.
Clinical outcomes are equivalent to EVLA; some studies show marginally less post-procedure bruising and discomfort with RFA.
- Ultrasound-Guided Foam Sclerotherapy (UGFS)
In this treatment a special medical-grade compound is injected into the affected veins that seals the leakage in the veins.
- Ambulatory Phlebectomy
This is one of the minimally invasive procedures used to remove superficial varicose veins through small punctures.
Performed under local anesthetic, this is often combined with ablation in the same session.
Source: ncbi (5)
Surgical Treatment for Varicose Veins Diseases
High Ligation and Stripping
This is a traditional surgical treatment for varicose veins. It carries higher complication rates than endovenous methods and involves longer recovery.
Ligation and stripping remain appropriate in specific anatomical situations or when other options are unavailable.
The treatment options are recommended only after a thorough examination; hence, it is advised to consult a professional.
Source: ncbi (6)
Recovery, Results & What to Expect After the Treatment
Recovery from modern minimally invasive procedures is generally very quick:
- Most patients walk immediately after the procedure
- Return to desk work: typically 1–2 days
- Return to exercise: usually 2–4 weeks depending on the procedure
- Compression stockings are worn for 1–2 weeks post-procedure in most protocols
- Bruising and mild tenderness along the treated vein is normal for 2–4 weeks
Conclusion
Varicose veins are far more than a cosmetic inconvenience. They are a manifestation of underlying venous malfunctioning that exists on a spectrum from minor surface vessels to advanced chronic venous insufficiency with skin and tissue damage.
The good news is that this is one of the most treatable conditions in vascular medicine.
Modern minimally invasive procedures offer excellent outcomes, minimal downtime, and high patient satisfaction.
Early assessment, accurate diagnosis with duplex ultrasound, and personalized treatment planning are the cornerstones of effective care.
If you have noticed prominent veins, are experiencing leg symptoms, or have a strong family history, the most important step is to seek an expert opinion.
A specialist vascular surgeon can assess your individual anatomy and advise on the best treatment option available for you.
FAQs
Can I treat varicose veins during pregnancy?
Treatment during pregnancy depends upon the trimester you’re in, although it is not recommended, but a specialist can give realistic advice depending on your condition.
Can Varicose Veins Be Prevented?
Yes, varicose veins diseases are preventable by taking small measures every day, like
- Staying active by regular walking, swimming, or cycling. This activates the calf pump and supports venous return.
- Maintaining a healthy weight reduces abdominal pressure on pelvic and leg veins.
- People with desk jobs can take movement breaks every 30–45 minutes when sitting or standing.
- If you have a family history, you can simply do a leg raise exercise for 20–30 minutes daily.
- Avoid hot baths and prolonged sun exposure, as they can worsen venous tone.
Does treatment hurt?
The modern treatment options are minimally invasive and are well tolerated by the patients.
Apart from this, post-procedure discomfort is typically manageable with over-the-counter analgesia.
Can diet affect varicose veins?
Diet does not cause or cure varicose veins directly, but anti-inflammatory, fiber-rich diets support vascular health and weight management.
Constipation (from low fiber intake) increases intra-abdominal pressure and straining, which raises venous pressure.
High sodium intake worsens edema. Adequate hydration supports blood viscosity.